An interview with Dr Mary Darking, University of Brighton
Homelessness and health are inextricably linked; experiencing homelessness, or risk of homelessness, can be devastating for a person’s health. The Brighton & Hove Common Ambition is a city-wide partnership project, with co-production at its heart, to improve Brighton & Hove’s health system for people experiencing homelessness.
In this interview to mark co-production week 2022 (4-9 July), Dr Mary Darking, Principal Lecturer at the University of Brighton (a Common Ambition partner), talks about the long term impact of co-production and how to ensure the project has a long-lasting, positive impact in the city of Brighton & Hove.

Mary Darking. Photo by Liz Finlayson/Vervate for Arch Healthcare
Q: How is Common Ambition working to ensure that co-production with people experiencing homelessness has a long-lasting effect on our city? How do we make sure co-production doesn’t just happen in silos and pockets but becomes part of how the city works?
Mary: Co-production is about putting lived experience at the centre of what we do. It is about committing to a process in which the intention at the outset is for that process to be led by people with lived experience.
When you go into co-production, your intention is to elevate the voices of people who aren’t ordinarily included or involved in important decisions, policy decisions, decisions about how services run, decisions about where people will be placed when they experience homelessness. That process of elevating voices is an ethical commitment. It shouldn’t be project-by-project, but rather, understood as fundamental to achieving positive system change. If we’re saying these voices have been absent, or not heard, then we’re saying that we need to change that systematically, not once in a while. What we have seen with Common Ambition is that when people have been marginalised and disadvantaged, historically, for so long and so completely, then it takes a lot of collaboration and trust building in the first instance to bring people to the room. In the case of people experiencing homelessness, they will have a lot going on in their lives; capacity to contribute to system change processes is a long way down the list. So, their commitment must be privileged and valued; it must be properly resourced and sustained. Because without lived experience voice, we are always going to miss the obvious. One of our lived experience Steering Group members said the other day; you can be an expert in something and engaged in it all the time, but if you have not lived through an experience, you miss the obvious. And that’s what lived experience brings; it is staggering how obvious the need for change can be when you actively listen to someone. It is getting people to listen – and then act – that is the challenge.

Photo by Liz Finlayson/Vervate for Arch Healthcare
Q: Could you tell me more about the work Common Ambition has done over the last year, in ensuring that there is a level playing field, where Steering Group members feel confident and empowered to play a central role in the project?
Mary: In this project we model what it is to be an ally to people who do not normally have the opportunity to speak and take decisions within innovation or system change projects. This is beyond consultation, user involvement or co-design. This is structurally, from the outset, designing decision-making structures that put people with lived experience at the centre. It is about elevating lived experience so that it is on a level playing field with all the other decision-makers and forms of knowledge in the room. Getting to that point where people are empowered and confident to be able to engage with system change takes time. In my view, this City needs to make a long-term, ethical commitment where we say ‘this is how it should be now’ and we ensure that co-production with people experiencing homelessness continues, beyond the life of a single project.
Q: Has there been any sort of discussion about the future within the Common Ambition lived experience steering group?
Mary: In setting up our Steering Group meetings our main concern as a group was to be trauma-informed. People are experiencing homelessness at the point they join the group. They have many more important concerns than our project to contend with. So together we have developed ways of reflecting on our work that help us see what we have done and where we are heading. That’s partly where our mapping process came from: week-by-week, we needed to see the picture build. We needed to retain what we were discovering, visually, in a way that we could all grasp again when we came to the next week’s meeting. For many of our members there have been meetings where they’ve not felt great, but they’ve come anyway. We offer support both in the meetings and through one-to-one follow-up to make sure everyone is okay. We know that thinking about planning three years work is really hard; it’s hard for a professional who is feeling well to do it. When life has been moment-to-moment, day-to-day, week-to-week, then envisaging the end of a long process can be too much. So, we think strategically, but also take things meeting by meeting. Working this way has been really positive and the group are clear that they are benefitting from this process; it’s been a personal journey for each of them. It’s not always been easy, but they have all described feeling more empowered, with meetings creating a sense of stability and purpose that they weren’t feeling previously. That’s fantastic, for those people who are in the room. What we need to do now is to think about who the next people are who are going to come through the door and how they can benefit from the skills and experience of their peers. This is why, collectively, we want to hold that long-term thinking at the forefront of our minds. It has to be a city that commits to these processes, not just one project; co-production needs to become a form of civic thinking. Otherwise, what happens to all the learning? What happens to the spaces that have been created for people to feel empowered to make these tremendous contributions about how to change the system, so that people can come through this experience with less ill-health and disability – and there is less death?
Q: As the project organisers, you and the team are holding both spaces: the project deadlines, and the thoughts about the longer term, ensuring that the city institutions are engaged, and ensuring they know what it means to move to this way of working.
Mary: We hold both spaces, but increasingly, as everyone learns new skills, we hold that space together, with our steering group members. We have our week-to-week meetings where the work happens, but we’re holding the longer term view as well. We hope the impact of this work will be a high-level recognition within health services that people who experience homelessness have far less capacity to have a voice. And if public patient involvement is an ethical commitment as well as a statutory requirement, then there needs to be recognition that patient public involvement for this group of people needs proper resourcing and supporting, otherwise we’ll never have those really vital feedback loops between people’s experiences of services and positive change.
We’ve seen this happening in so many other areas of health care; there are so many other really strong, really amazing patient groups, advocates, charities and organisations. It’s a vital part of the care ecosystem, that people can organise to make their voices heard. In that respect, people experiencing homelessness are at a profound disadvantage compared to other patient groups.
Q: Could you tell me any more about working with the city institutions and ensuring that there is city-wide buy in, and longer-term support?
Mary: If this is a real co-production process, eventually it needs to be a process that people with lived experience own. It needs a structure to enable it to stand on its own two feet and have its ideas and initiative valued, with a genuine sense of ally-ship from other organisations. So the ultimate end point would be that people with lived experience own the co-production process itself, and the means through which it’s organised, and that they can turn to people and institutions in the city for support, and those people come willingly alongside them.
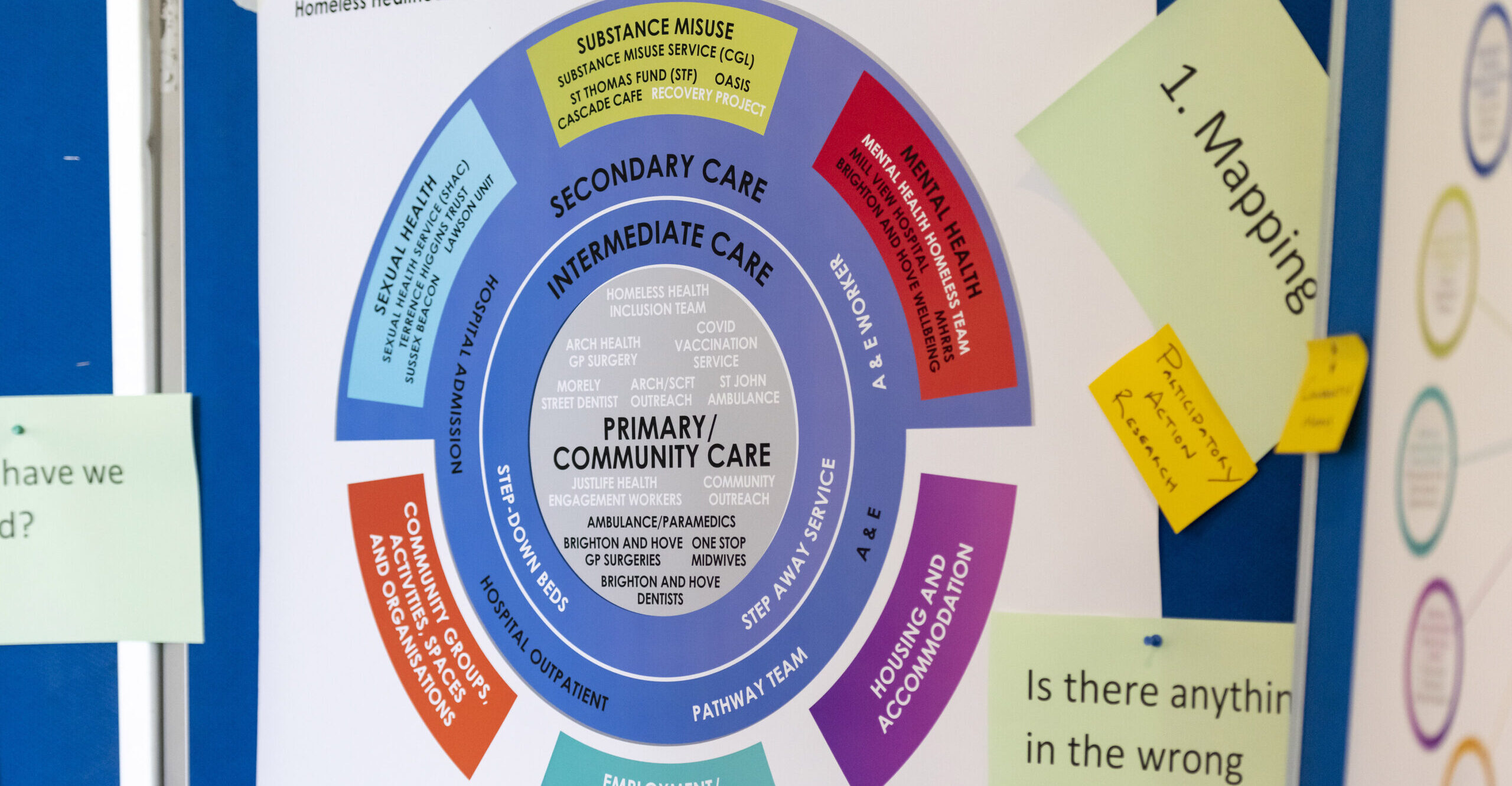
Photo by Liz Finlayson/Vervate for Arch Healthcare
Q: How do you see this structure looking in the long term?
Mary: It could perhaps be envisaged as a sort of peer learning group where there are people with lived experience who have been through this system change process, can pass that knowledge and learning on to others and support them through the empowerment journey that they themselves have been through, making sure it doesn’t get too static. You would need to ensure there was a constant flow of people who are being heard and who are benefiting from the experience. And that’s quite difficult to achieve. A helpful model might be an adult education or training and development space. But it could just as easily be a social movement.
Q: Do you know of any examples where this way of working has been successful?
Mary: There is Oxfordshire’s Lived Experience Advisory Forum (LEAF), which has been framed as a social movement, as a conversation between people experiencing homelessness and the city. However, the health dimension of Common Ambition is really important: having a voice within NHS systems. Good system change can happen if patient voices are heard.
Q: Do you think there’s anything particular to Brighton and Hove that means that our city might be an especially good place to get this sort of change started?
Mary: The existing innovation we have in homeless healthcare systems in the city is an excellent platform to be starting from. It means that we have already got clinicians who have chosen to specialise in this field and are driving innovation forward. And it means that you’ve already got commissioners and public health partners who are knowledgeable and ready to take innovation forward. We also have a tremendous third sector and Brighton and Hove. Their recent report shows what an amazing job they do in the city.
From residents of Brighton and Hove there is also a strong civic energy. In the winter of 2018, a Brighton University researcher mapped all the different grassroots groups that formed to address rough sleeping. It showed a huge amount of grassroots, civic commitment and concern about homelessness. A large-scale survey went out a few years ago for the Fairness Commission. There were just two questions: What can we do to make Brighton and Hove a fairer city? And what can you do to make Brighton and Hove for a fairer city? By far the most reported response, across the board, was: end homelessness.
I think as a city, we have a strong sense of fairness and justice. It affects people deeply to see other people clearly suffering; clearly not receiving the support and housing options they need. People with lived experience of homelessness will tell you this must end. Our job is to join our voices with theirs in demanding that it does.